Lipiodol chemoembolization for colorectal cancer: An in vivo animal study and a preliminary clinical study

Introduction: Colorectal cancer (CRC) is the third most common cancer worldwide.
Objective: This study aims to investigate the safety and effectiveness of Lipiodol chemoembolization (LCE) of the colorectal artery in an in vivo animal study and a retrospective clinical study in patients with advanced CRC.
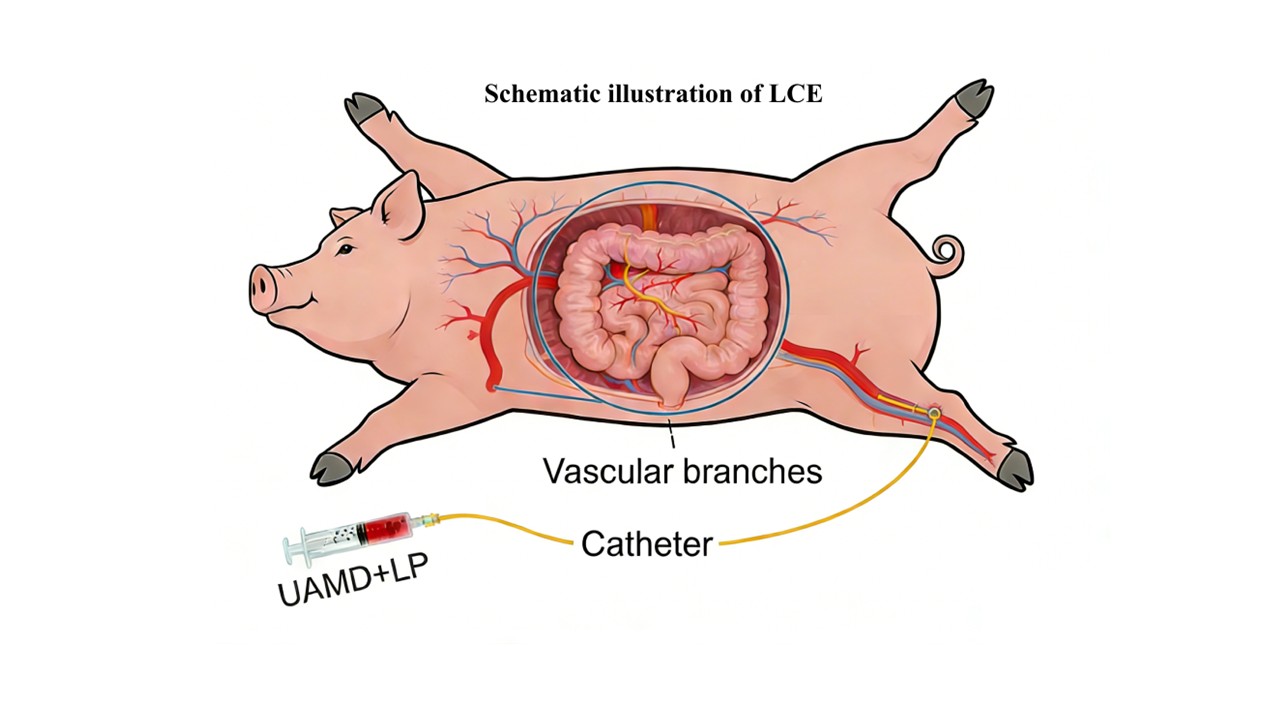
Methods: The in vivo study was conducted on six Large White pigs undergoing LCE of the posterior mesenteric artery. Lipiodol distribution in the colorectal tract was observed using computed tomography. Colonoscopy and pathological examinations were used to evaluate mucosal reactions. For the preliminary clinical study, 12 patients with advanced CRC received LCE. Subsequently, procedure-related complications, adverse reactions, and tumor changes after iodized oil embolization were observed.
Results: Following chemoembolization, no severe complications (e.g., necrosis, perforation) were observed in pigs. Acute colorectal edema detected on post-operative day 1 resolved progressively, with complete clearance of Lipiodol by day 14. Pathological manifestations included mucosal and submucosal infiltration of neutrophils, lymphocytes, macrophages, and other inflammatory cells, focal mild erythrocyte extravasation, local mucosal erosion, and superficial ulceration—all of which resolved completely on follow-up. No peri-procedural severe adverse events occurred in patients. Transient mild abdominal pain, mucinous discharge, and tenesmus were common but improved rapidly. The overall disease control rate and objective response rate were 91.6% and 83.3%, respectively. Disease stage and post-treatment systemic therapy were significant predictors of overall survival (OS). The median OS was 16.0 months (95% confidence interval: 14.51–25.65).
Conclusion: LCE of the colorectal artery appears to be technically feasible and safe. It may be considered a potential novel treatment option for patients with advanced CRC.
- Siegel RL, Miller KD, Wagle NS, Jemal A. Cancer statistics, 2023. CA Cancer J Clin. 2023;73(1):17-48. doi: 10.3322/caac.21763
- Fuentes Bayne HE, Suleiman R, Eiring RA, et al. CDX2 expression as a predictive and prognostic biomarker of 5-FU response in cancer of unknown primary. ESMO Open. 2025;10(8):105515. doi: 10.1016/j.esmoop.2025.105515
- Chan WY, Chua W, Wilkinson K, et al. The prognostic and predictive utility of CDX2 in colorectal cancer. Int J Mol Sci. 2024;25(16):8673. doi: 10.3390/ijms25168673
- Badia-Ramentol J, Gimeno-Valiente F, Durendez E, et al. The prognostic potential of CDX2 in colorectal cancer: Harmonizing biology and clinical practice. Cancer Treat Rev. 2023;121:102643. doi: 10.1016/j.ctrv.2023.102643
- Bray F, Laversanne M, Sung H, et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2024;74(3):229-263. doi: 10.3322/caac.21834
- Osseis M, Nehmeh WA, Rassy N, et al. Surgery for T4 colorectal cancer in Older patients: Determinants of outcomes. J Pers Med. 2022;12(9):1534. doi: 10.3390/jpm12091534
- Chakedis J, Schmidt CR. Surgical treatment of metastatic colorectal cancer. Surgical Oncol Clin N Am. 2018;27(2):377-399. doi: 10.1016/j.soc.2017.11.010
- Zacharakis M, Xynos ID, Lazaris A, et al. Predictors of survival in stage IV metastatic colorectal cancer. Anticancer Res. 2010;30(2):653-660.
- Feria A, Times M. Effectiveness of standard treatment for stage 4 colorectal cancer: Traditional management with surgery, radiation, and chemotherapy. Clin Colon Rectal Surg. 2023;37(2): 62-65. doi: 10.1055/s-0043-1761420
- Yang T, Guo L. Advancing gastric cancer treatment: Nanotechnology innovations and future prospects. Cell Biol Toxicol. 2024;40(1):101. doi: 10.1007/s10565-024-09943-9
- Alrushaid N, Khan FA, Al-Suhaimi E, Elaissari A. Progress and perspectives in colon cancer pathology, diagnosis, and treatments. Diseases. 2023;11(4):148. doi: 10.3390/diseases11040148
- Zellweger M, Abdelnour-Berchtold E, Krueger T, Ris HB, Perentes JY, Gonzalez M. Surgical treatment of pulmonary metastasis in colorectal cancer patients: Current practice and results. Crit Rev Oncol Hematol. 2018;127:105-116. doi: 10.1016/j.critrevonc.2018.05.001
- Dominguez OH, Yilmaz S, Steele SR. Stage IV colorectal cancer management and treatment. J Clin Med. 2023;12(5):2072. doi: 10.3390/jcm12052072
- Turk PS, Belliveau JF, Darnowski JW, Weinberg MC, Leenen L, Wanebo HJ. Isolated pelvic perfusion for unresectable cancer using a balloon occlusion technique. Arch Surg. 1993;128(5):533-8, discussion 538-9. doi: 10.1001/archsurg.1993.01420170067009
- Woeste MR, Philips P, Egger ME, Scoggins CR, McMasters KM, Martin RCG. Optimal perfusion chemotherapy: A prospective comparison of mitomycin C and oxaliplatin for hyperthermic intraperitoneal chemotherapy in metastatic colon cancer. J Surg Oncol. 2020;121(8):1298-1305. doi: 10.1002/jso.25920
- Symer MM, Wong NZ, Abelson JS, Milsom JW, Yeo HL. Hormone replacement therapy and colorectal Cancer incidence and mortality in the prostate, lung, colorectal, and ovarian Cancer screening trial. Clin Colorectal Cancer. 2018;17(2):e281-e288. doi: 10.1016/j.clcc.2018.01.003
- Modest DP, Pant S, Sartore-Bianchi A. Treatment sequencing in metastatic colorectal cancer. Eur J Cancer. 2019;109:70-83. doi: 10.1016/j.ejca.2018.12.019
- Abdul-Latif M, Townsend K, Dearman C, Shiu KK, Khan K. Immunotherapy in gastrointestinal cancer: The current scenario and future perspectives. Cancer Treat Rev. 2020;88:102030. doi: 10.1016/j.ctrv.2020.102030
- Martinez-Castedo B, Camblor DG, Martin-Arana J, et al. Minimal residual disease in colorectal cancer. Tumor-informed versus tumor-agnostic approaches: Unraveling the optimal strategy. Ann Oncol. 2024;36(3):263-276. doi: 10.1016/j.annonc.2024.12.006
- Chidharla A, Rapoport E, Agarwal K, et al. Circulating tumor DNA as a minimal residual disease assessment and recurrence risk in patients undergoing curative-intent resection with or without adjuvant chemotherapy in colorectal cancer: A systematic review and meta-analysis. Int J Mol Sci. 2023;24(12):10230. doi: 10.3390/ijms241210230
- Bua-Ngam C, Norasetsingh J, Treesit T, et al. Efficacy of emergency transarterial embolization in acute lower gastrointestinal bleeding: A single-center experience. Diagn Interv Imaging. 2017;98(6):499-505. doi: 10.1016/j.diii.2017.02.005
- Hur S, Jae HJ, Lee M, Kim HC, Chung JW. Safety and efficacy of transcatheter arterial embolization for lower gastrointestinal bleeding: A single-center experience with 112 patients. J Vasc IntervRadiol. 2013;25(1):10-19. doi: 10.1016/j.jvir.2013.09.012
- Pannatier M, Duran R, Denys A, Meuli R, Zingg T, Schmidt S. Characteristics of patients treated for active lower gastrointestinal bleeding detected by CT angiography: Interventional radiology versus surgery. Eur J Radiol. 2019;120:108691. doi: 10.1016/j.ejrad.2019.108691
- Seyferth E, Dai R, Ronald J, et al. Safety profile of particle embolization for treatment of acute lower gastrointestinal bleeding. J Vasc Interv Radiol. 2021;33(3):286-294. doi: 10.1016/j.jvir.2021.11.006
- Frost J, Sheldon F, Kurup A, Disney BR, Latif S, Ishaq S. An approach to acute lower gastrointestinal bleeding. Frontline Gastroenterol. 2015;8(3):174-182. doi: 10.1136/flgastro-2015-100606
- Hosse C, Moos M, Becker LS, et al. Trans-arterial embolization for treatment of acute lower gastrointestinal bleeding-a multicenter analysis. European Radiology. 2024;35(5):2746-2754. doi: 10.1007/s00330-024-11102-x
- De Baere T, Dufaux J, Roche A, et al. Circulatory alterations induced by intra-arterial injection of iodized oil and emulsions of iodized oil and doxorubicin: Experimental study. Radiology. 1995;194(1):165-170. doi: 10.1148/radiology.194.1.7997545
- Pillai K, Ke K, Mekkawy A, Akhter J, Morris DL. Enhancement of treatment efficacy of hepatic tumours using Trans-arterial-chemoembolization. Am J Cancer Res. 2023;13(5):1623-1639.
- European Association for the Study of the Liver, European Organisation For Research and Treatment of Cancer. EASL-EORTC clinical practice guidelines: Management of hepatocellular carcinoma. J Hepatol. 2012;56(4):908-943. doi: 10.1016/j.jhep.2011.12.001
- Idee JM, Guiu B. Use of Lipiodol as a drug-delivery system for transcatheter arterial chemoembolization of hepatocellular carcinoma: A review. Crit Rev Oncol Hematol. 2013;88(3):530-549. doi: 10.1016/j.critrevonc.2013.07.003
- Zhang J, Li X, Yin M, et al. Transarterial infusion chemotherapy combined with iodinated oil chemoembolization for the treatment of primary colorectal cancer. J Cancer Res Ther. 2025;21(6):1221-1226. doi: 10.4103/jcrt.jcrt_2515_24
- Gonsalves CF, Brown DB. Chemoembolization of hepatic malignancy. Abdom Imaging. 2009;34(5):557-565. doi: 10.1007/s00261-008-9446-y
- Plakhotnyi RО, Кerechanyn ІV, Fedoniuk LY, Kovalchuk NV, Dehtiariova OV, Singh G. Comperative structure of mucosa coat of the pig`s and the human`s rectum. Wiad Lek. 2021;74(7):1718-1721.doi: 10.36740/wlek202107128
- Anteby R, Kemeny NE, Kingham TP, et al. Getting chemotherapy directly to the liver: The historical evolution of Hepatic Artery chemotherapy. J Am Coll Surg. 2020;232(3):332-338. doi: 10.1016/j.jamcollsurg.2020.11.013
- Kan Z, Sato M, Ivancev K, et al. Distribution and effect of iodized poppyseed oil in the liver after hepatic artery embolization: Experimental study in several animal species. Radiology. 1993;186(3):861-866. doi: 10.1148/radiology.186.3.8381552
- Kan Z, Ivancev K, Hagerstrand I, Chuang VP, Lunderquist A. In Vivo Microscopy of the liver after injection of lipiodol into the hepatic artery and portal vein in the rat. Acta Radiologica. 1989;30(4):419-425. doi: 10.1177/028418518903000418
- Caine M, Chung T, Kilpatrick H, et al. Evaluation of novel formulations for transarterial chemoembolization: Combining elements of lipiodol emulsions with drug-eluting beads. Theranostics. 2019;9(19):5626-5641. doi: 10.7150/thno.34778
- Grosskinsky CM, Clark RL, Wilson PA, Novotny DB. Pelvic granulomata mimicking endometriosis following the administration of oil-based contrast media for hysterosalpingography. Obstet Gynecol. 1994;83(5 Pt 2):890-892.
- Miyazaki Y, Yamamoto T, Hyakudomi R, et al. Case of inflammatory granuloma in inguinal hernia sac after hysterosalpingography with oily contrast medium. Int J Surg Case Rep. 2020;72:215-218. doi: 10.1016/j.ijscr.2020.05.084
- Golfieri R, Renzulli M, Mosconi C, et al. Hepatocellular carcinoma Responding to superselective transarterial chemoembolization: An issue of nodule dimension? J Vasc Interv Radiol. 2013;24(4):509-517. doi: 10.1016/j.jvir.2012.12.013
- Miyayama S, Matsui O. Superselective Conventional Transarterial chemoembolization for hepatocellular carcinoma: Rationale, technique, and outcome. J Vasc Interv Radiol. 2016;27(9):1269-1278. doi: 10.1016/j.jvir.2016.04.014
- Yamakado K, Miyayama S, Hirota S, et al. Hepatic arterial embolization for unresectable hepatocellular carcinomas: Do technical factors affect prognosis? Jpn J Radiol. 2012;30(7):560-566. doi: 10.1007/s11604-012-0088-1
- Goseki N, Nosaka T, Endo M, Koike M. Nourishment of hepatocellular carcinoma cells through the portal blood flow with and without transcatheter arterial embolization. Cancer. 1995;76(5):736-742. doi: 10.1002/1097-0142(19950901)76:5
- Kan Z, Madoff DC. Liver anatomy: Microcirculation of the liver. Semin Interv Radiol. 2008;25(2):77-85. doi: 10.1055/s-2008-1076685
- Llovet JM, Real MI, Montana X, et al. Arterial embolisation or chemoembolisation versus symptomatic treatment in patients with unresectable hepatocellular carcinoma: A randomised controlled trial. Lancet. 2002;359(9319):1734-1739. doi: 10.1016/s0140-6736(02)08649-x
- Brown DB, Pilgram TK, Darcy MD, et al. Hepatic arterial chemoembolization for hepatocellular carcinoma: Comparison of survival rates with different embolic agents. J Vasc Interv Radiol. 2005;16(12):1661-1666. doi: 10.1097/01.rvi.0000182160.26798.a2
- Hao MZ, Lin HL, Chen QZ, et al. Safety and efficacy of transcatheter arterial chemoembolization with embospheres in treatment of hepatocellular carcinoma. J Dige Dis. 2016;18(1):31-39. doi: 10.1111/1751-2980.12435
- Ensminger WD, Gyves JW. Clinical pharmacology of hepatic arterial chemotherapy. Semin Oncol. 1983;10(2):176-182.
- Ensminger WD, Rosowsky A, Raso V, et al. A clinical-pharmacological evaluation of hepatic arterial infusions of 5-fluoro-2’-deoxyuridine and 5-fluorouracil. Cancer Res. 1978;38(11 Pt 1):3784-3792.

